Health, Pickleball, Tennis
Welcome and thanks for visiting...

What Is Plantar Fasciitis?
We have all heard of it, and some of us have even experienced it. Plantar Fasciitis. What is it, and how do we treat it? Before we go there, we should first take a look at the foot, what the plantar fascia is, and what function it has. The human foot is a complex structure composed of 26 bones, 33 joints, and over 100 muscles. The complexity of the structure is due to the necessity of the function of the foot. The foot is the first shock absorber in the system when walking, running, or jumping. Anytime the foot contacts the ground, it is the first shock absorber in the system. If the foot is not articulating (moving) as it should, this means that less force is absorbed, which aids in increased risk for injury. With normal daily activities, the force the foot must absorb ranges from 1 (walking) to 4 times (descending stairs) body weight. With sporting activities, this can range from 4 to 8 times body weight depending on the activity and the playing surface. Obviously, this is a lot of force to absorb, and the efficiency of the first shock absorber in the system is essential. If less force is absorbed, then this force is transmitted to the knee, hip, and lower back. This is one reason that people who suffer chronic foot problems often end up developing knee pain, hip pain, or lower back pain on that same side.
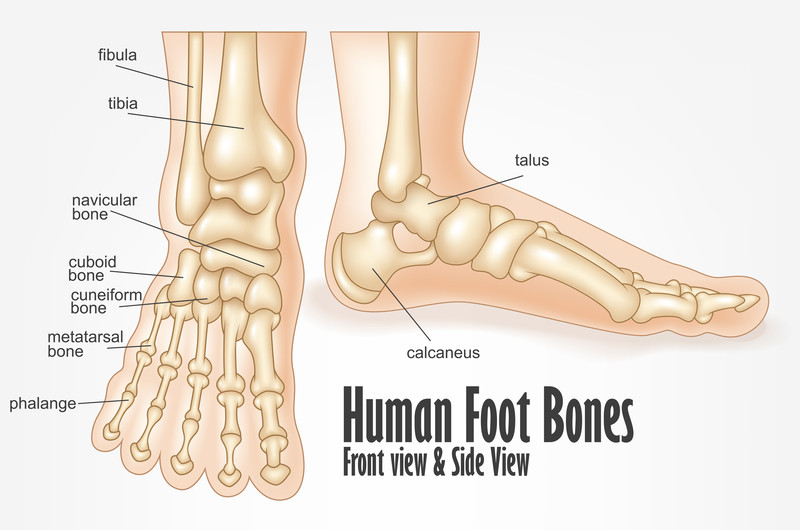
The foot is designed for this shock-absorbing function. When walking, the general pattern of movement of the foot is the heel, which is the first thing that comes into contact with the ground. The design of the fat pad on the heel, the concentric rings of the fat pad, is specifically designed to compress and aid in the absorption of force in the heel. This function prevents bone bruising of the calcaneus or heel. With time (age) these tissues become less resilient, loose some of the compressive capability and can be one reason people start to develop heal pain. As you proceed with your walking, after the heel has contacted the ground, your foot rolls out slightly (supinates) toward your small toe as you proceed to mid-stance, then rolls in (pronates) to push off on the big toe. The big toe is a much bigger bone than the other bones, so it can absorb this force as it bears a majority of the weight at the toe.
With the foot moving in this fashion and the fact that it has 33 joints and 30+ ligaments, this motion of the joints, the stretching of the ligaments, and the contraction of the 100-plus muscles of the foot and ankle allows greater absorption of force and hence reduces the risk of that excessive force being transferred up the chain to the knee, hip and low back. On the bottom of the foot, the structures that aid in shock absorption are a tissue on the underside of the foot called the plantar fascia and the intrinsic muscles of the foot (abductor halluces, the flexor digitorum brevis, the abductor digiti minimi, and the quadratus plantae).
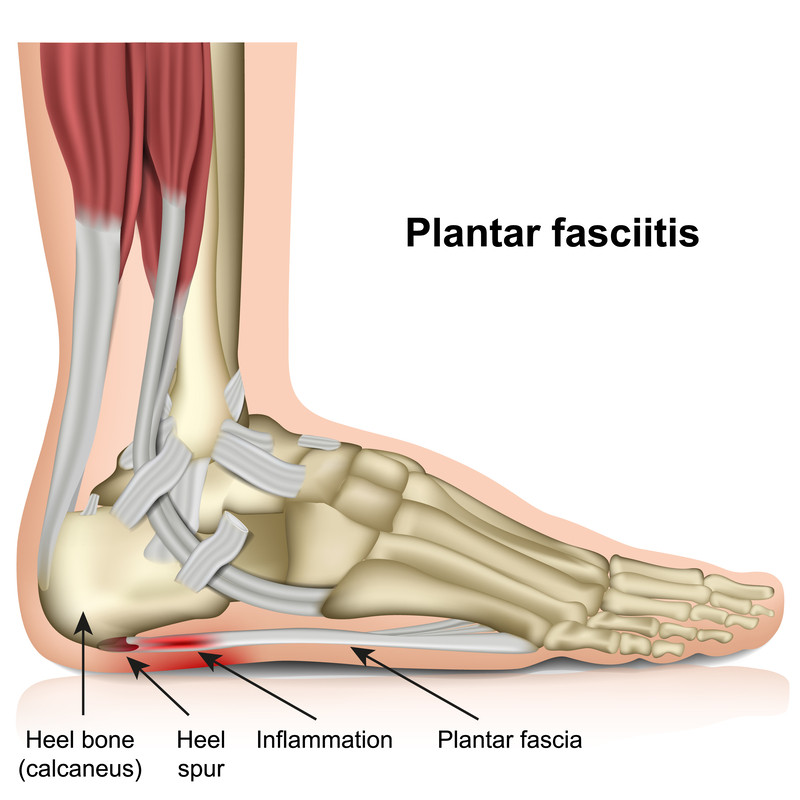
The plantar fascia
The plantar fascia is a thick fibrous tissue that stretches from the calcaneus (heel) to the toes and end of the first toe. When looking closely at the anatomy of the plantar fascia, you see that the gastrocnemius (calf) attaches to the heel via the Achilles tendon. The Achilles tendon or fibers of (fascia) continue over the bottom of the calcaneus to become the plantar fascia. As the foot goes through the motions described above, the arch of the foot wants to collapse. The plantar fascia, through its elasticity, stretches and prevents the arch from collapsing and, at the same time, absorbs the kinetic energy with this stretching function.

The origin and attachments of the plantar fascia are important because this has a huge impact on stretching both the plantar fascia and the Achilles tendon. Knowing that fibers of the Achilles tendon continue on to become the plantar fascia means we can facilitate a much better stretch by getting an extension of the first ray (toe), plantar fascia, and calf, all stretching at the same time. Creating flexibility along this entire complex helps and aids in preventing plantar fasciitis, Achilles tendonitis/tear, and calf strains. The more elasticity this tissue has, the more it can be stretched and absorb energy without becoming overstretched and irritated. The stretch pictured here has the athlete getting an extension of the first ray and stretch to the plantar fascia and calf. If she keeps her knee straight and drives toward the wall, this will stretch the gastrocnemius, and if she bends her knee and drives toward the wall, this will stretch her soleus (also a calf muscle). Both of these will also stretch the plantar fascia.
In the next blog, we will discuss more about plantar fasciitis and how to prevent it. Stay tuned.
Read more:






