Health, Regeneration
Welcome and thanks for visiting...

Do You Know What You Need to Know About Stress Fractures?

Understanding the basic science of the skeletal system may affect your athletes in a positive way whether you are a coach or a parent. The previous blog post “Let’s Give the Skeleton the Focus it is Due” gave an overview of the importance of skeletal training and some unique features of that training. Now we will focus on stress fractures and how a basic understanding of the bone remodeling process will provide a perspective that coaches, parents, and athletes can use to help prevent stress fractures and optimize recovery when they do occur. The key points highlighted below come from my students in Kin 409 Bone and Exercise in the Department of Kinesiology at Cal State East Bay.
By the Numbers.
Stress fractures sideline many athletes each year with women’s cross-country, gymnastics, outdoor track, and men’s cross-country having the highest incidence. Almost a quarter of stress fractures are recurrent with women’s field hockey having a 36.4% recurrence rate, women’s gymnastics at 34.6% and 26.3% for women’s outdoor track. The predominant areas that athletes experience stress fractures include the lumbar spine/pelvis, the femur and tibia (leg bones) and the navicular and metatarsals (bones in the foot). Furthermore, female athletes are more likely than their male counterparts to develop stress fractures with significantly higher rates (9.13/100,000 athlete exposures) compared to males (4.44/100,000 athlete exposures) (An athletic exposure is a game or a practice). These stats are based on a 2017 article summarizing NCAA (National Collegiate Athletic Association) injury surveillance data survey from academic years 2004-05 through 2013-14 (Rizzone et al., 2017).
High school athletes are also at risk. Injury data is compiled from all US High Schools with a Certified Athletic Trainer (ATC) affiliated with the National Athletic Trainers Association (NATA) (Note: parents and coaches should make sure their high school athletes have a certified ATC on staff). Data are collected via the High School Reporting Information Online (RIO), an internet-based sports injury surveillance system started at the Center for Injury Research and Policy at Nationwide Children's Hospital. The overall rate of stress fracture was 1.54/100,000 athlete exposure. Of the total number of injuries reported from 2005-06 through 2012-13, 0.8% were stress fractures. Girls sustained more stress fractures (63.3%) compared with boys (36.7%) and sports with the highest rates were girls’ cross-country with a rate of 10.62/100,000 athlete exposure, girls’ gymnastics at 7.43/100,000 athlete exposure and boys cross-country at 5.42/100,000 athlete exposure. Common sites for high school athletes are similar to collegiate athletes, the lower leg at 40.3%, 34.9% of the injuries at the foot and 15.2% in the lower back/ lumbar spine/pelvis. It is important to appreciate that stress fractures can require long recovery times, 65.3% of athletes had more than 3 weeks of lost time in their sport or the injury ended their season.
So, what is a stress fracture?
Stress fractures now commonly called bone stress injuries (BSI) are NOT acute injuries where the athlete falls down and grabs their leg in pain, but these injuries occur on a continuum and are associated with repeated loading and inadequate recovery. The key factor contributing to stress fracture is repetitive loading, simply stated our bones get
micro cracks during use which are typically repaired but when the repair process cannot keep up with the injury then the BSI continuum will progress. Typically, we think of runners when talking about BSI/stress fracture injuries however volleyball and basketball players also have a high incidence of injury.
The BSI continuum starts as a stress reaction, the athlete feels localized pain and tenderness when pressing on the affected area. The pain then gets worse as the athlete continues activity and can progress to a stress fracture which is a small crack in the bone. The athlete may feel a dull ache near site with potential swelling that results in an increase in pain when weight bearing even when just walking. As the injury progresses there is more of a mismatch between damage in the bone from the repetitive loading and the recovery process which is called bone remodeling.
What is Bone Remodeling?
To really understand the cause of BSI’s it's helpful to understand some of the basic physiology of bone. First, let's review the two of the three cells in bone, osteoblasts, and osteoclasts.
Osteoblasts make bone and osteoclasts break down bone, these cells tend to work together replacing older bone or repairing injured bone. In fact, every 7 years we have a new skeleton as a result of the osteoblasts and osteoclasts working together in a process called remodeling.

Remodeling is a process that is ongoing in the body; the osteoclasts take away injured bone and osteoblasts lay down new bone to complete the repair process. It is important to note that there is a time lag both between the activity of breaking down bone from the osteoclasts and making new bone from the osteoblasts as well as time is needed for new bone to become sufficiently strong by completely mineralizing. Similar to painting a room in your home, there is a time lag between painting the walls and letting them dry and moving furniture back in and using that room.
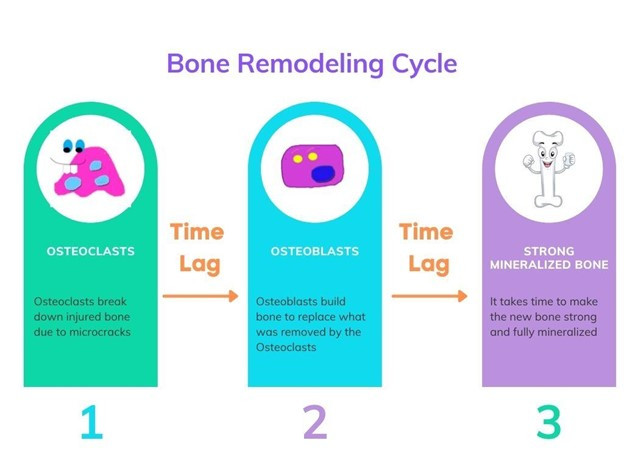
Recovery Approach from Bone Strain Injuries (BSI’s)
One suggestion for recovery from a BSI is the acronym REST (Romani et al., n.d.)
Removing activity
Exercise to maintain fitness
Safe and pain free return to previous activity
Time for new bone to mature and catch up with remodeling.
The T in the REST approach considers the lag between osteoclast and osteoblast activity and the time lag for bone mineralization. Following injury, as an athlete begins to increase their training back to normal activity levels, rest days need to be integrated in order for the remodeling process to be effective in “healing” the BSI. In fact, some suggest having an entire rest week, about 3 weeks after an increase in training load based on the bone remodeling cycle. Further support for this approach comes from research in military recruits, BSIs begin appearing approximately 3 weeks into basic training (Armstrong et al., 2004). Planning rest days and weeks may optimize an athletes return to play after suffering a BSI.
Can we PREVENT BSI’s?
Eating a balanced diet, sleeping well and proper footwear can help athletes stay healthy. But training factors are the key contributors to developing BSI’s and ultimately stress fractures. Rapid increases in training load such as those during pre-season result in an increased incidence of BSI’s but optimized training approaches that include rest periods may help to avoid the onset of the BSI continuum.
While there are no definitive ways to predict, prevent or rehabilitate BSI’s/stress fractures, understanding bone remodeling and good communication between coaches, parents and rehabilitation specialists may go a long way in keeping our athletes in the game.
TAKE HOME POINTS
- BSI’s/Stress fractures occur in female athletes at a greater rate than male athletes
- Key sports affected: women’s and men's cross-country, women’s gymnastics and women's outdoor track
- Bone Stress Injury (BSI) is a continuum so catching the injury early in the process can prevent an ACTUAL stress fracture.
- Week 3 after increasing training load seems to be a vulnerable time point for the skeletal system. The remodeling cycle is responsible for “healing” bone but since there is a time lag between breaking down bone and building bone and mineralization there is a period of time that bones may be relatively “weak” during this process. Be mindful of the lag when reintroducing athletes back to practice and competition.
- Each athlete is different, NO one size fits all works for recovery
References:
Armstrong, D. W., Rue, J.-P. H., Wilckens, J. H., & Frassica, F. J. (2004). Stress fracture injury in young military men and women. Bone, 35(3), 806–816. https://doi.org/10.1016/j.bone.2004.05.014
Rizzone, K. H., Ackerman, K. E., Roos, K. G., Dompier, T. P., & Kerr, Z. Y. (2017). The Epidemiology of Stress Fractures in Collegiate Student-Athletes, 2004–2005 Through 2013–2014 Academic Years. Journal of Athletic Training, 52(10), 966–975. https://doi.org/10.4085/1062-6050-52.8.01
Romani, W. A., Gieck, J. H., Perrin, D. H., Saliba, E. N., & Kahler, D. M. (n.d.). Mechanisms and Management of Stress Fractures in Physically Active Persons. 9.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC164361/





